What to know about Candida when you have Mast Cell Activation Syndrome | Histamine Intolerance
Many of us with Mast Cell Activation Syndrome and Histamine Intolerance deal with Candida issues.
For me, I started getting vaginal yeast infections when I was a teenager. They were really uncomfortable! And honestly, embarrassing. Particularly because they continued into my late 20s.
I was getting 5-6 yeast infections a year – yuck!!
I also developed a type of skin yeast infection called tinea versicolor. It causes dark (or sometimes light) patches on the skin. They looked pretty weird.
I also had a lot of gut problems, like bloating, cramping and loose stools.
These were all major signs of some major underlying problems. But, it took years to sort out.
When I stopped eating sugar and junk carbs, the vaginal yeast infections went away. But the dark patches from the skin yeast infection required a couple courses of antifungal cream to get rid of.
Why was this happening to me? Even though it’s hard to write about these things (and especially post online!), I wanted you to know you’re not alone in this.
Especially if you have Mast Cell Activation Syndrome or Histamine Intolerance.
I want to share with you all kinds of details about Candida, specifically for people with Mast Cell Activation Syndrome and Histamine Intolerance. And more about the problems underlying Candida if you’re dealing with it.
Let’s first look at what Candida is…
Introduction to Candida
So, to get started, what is Candida? Candida albicans is a fungal species that naturally grows in the body.
When we talk about “getting candida” or “having candida,” we’re really referring to an overgrowth of Candida albicans.
A candida overgrowth or infection is also called Candidiasis.
How do people get a Candida overgrowth? Candida overgrowth can be triggered by a number of things:
- High insulin/high sugar diet
- Steroids like Prednisone
- Antibiotics
- Birth control pills
- Cancer treatments
- A wonky (dysregulated) immune system – either underactive or overactive
But the BIGGEST reason for Candida issues is Mold Toxicity. Mold can make it where your immune system can’t keep things like Candida in check anymore.
We’ll talk about this more in a bit.
Candida Overgrowth Can Trigger Mast Cell Activation Syndrome and Histamine Intolerance
The way it does this is the same with any type of infection. When candida overgrows, it triggers an immune response.
Once the immune system is triggered, there is a release of histamine and other inflammatory molecules.
In addition, some people develop IgE and IgG antibodies to Candida. That can make their reactions to candida even worse.
Candida overgrowth can show up in these areas of the body:
- GI tract
- Vaginal canal
- External genitals
- Mouth
- Skin
- Lungs, but that’s more rare
It’s important to remember that Candida is a normal part of your gut. We actually need a good balance of Candida for healthy immunity.
In fact, recent studies have shown that Candida in proper balance may help with autoimmunity.
But it’s tricky, because allergy responses to Candida can also be a big issue in Mast Cell Activation Syndrome.
Especially in Mold Toxicity. Again, the key is the right balance.
How do you know if you are dealing with candida overgrowth?
Certain symptoms can clue you in. We’ll cover that next…
How To Know If You are dealing With Candida
There are a number of symptoms that can be clues you’re dealing with candida overgrowth, like
- Sugar cravings
- Chronic sinus congestion and allergies
- Urinary Tract Infection (UTI)
- Vaginal yeast infections
- White patches inside the mouth (including canker sores)
- White coating on tongue
- Bad breath
- Dandruff
- Athlete’s foot
- Toenail fungus
Candida produces these symptoms by disrupting the healthy balance of bacteria in these areas. Candida can also cause these kinds of symptoms through inflammation and the immune response.
Here’s how that happens…
Cells, like the mast cells, realize there’s some major overgrowth going on. So, it sends out the immune first responders called white blood cells.
When there’s an infection or overgrowth of any sort, white blood cells are sent to the area of irritation or tissue damage.
That leads to mucus production and sometimes scabbing. And can cause the types of symptoms you saw above.
Guess what else usually goes along with Candida?
Mold.
And mold can work with candida to keep you sick.
Plus, mold also creates Candida issues.
Want to know how? The mold-candida connection is coming up next.
The Mold – Candida Connection
If you have a chronic mold issue, it’s very hard to get rid of candida. For some people, it’s almost impossible until the mold is gone.
This is because mold blocks the killing side of the immune system. This makes it harder to keep candida and other species in check in the gut.
Another big reason is because if you have mold issues, that mold produces oxalates. And oxalates feed candida.
Stubborn candida cases nearly always have underlying Mold Toxicity.
See, molds make certain toxins that can cause significant Mast Cell Activation. And further weaken the immune system against mold.
According to studies, Candida can likely also make Gliotoxin. And this Gliotoxin is another way Candida can make people feel really bad.
You can learn more about Mold Toxicity by reading these blog posts:
- Mycotoxins and Mold: One of the Biggest Root Triggers for Mast Cell Activation | Histamine Intolerance
- How To Detox Your Body from Mold with MCAS
- Top Tips on Environmental Mold for those with Mast Cell Activation Syndrome and Histamine Intolerance
But, how do you know if you have candida overgrowth? Are there tests for this? We’ll talk about some testing options next.
Testing for Candida
To find out whether you’re dealing with a candida infection, there are a couple of different tests you can do.
One option is to get a Great Plains Microbial Organic Acid Test. You can order it on your own with that link. The results will include fungal and candida markers.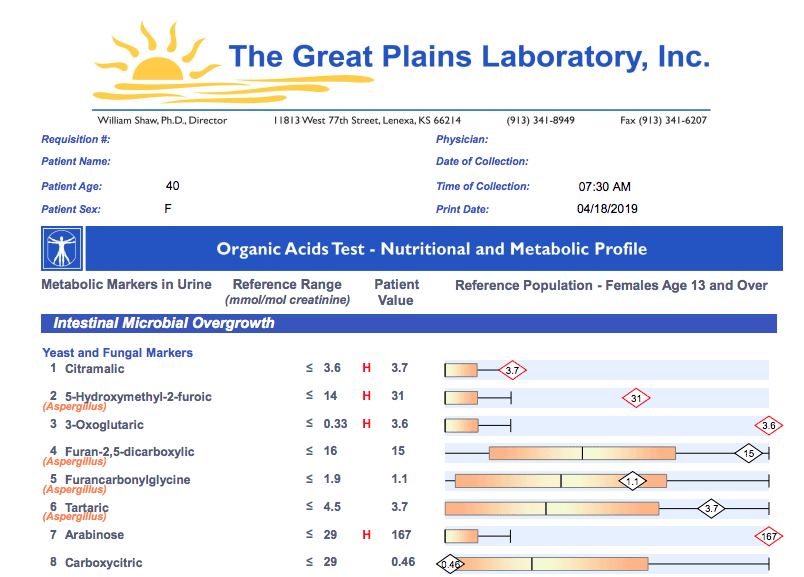
- A second option is to order the full Organic Acid Test. The results of this test include all the fungal and candida markers. And also markers for oxalates plus dozens more markers.
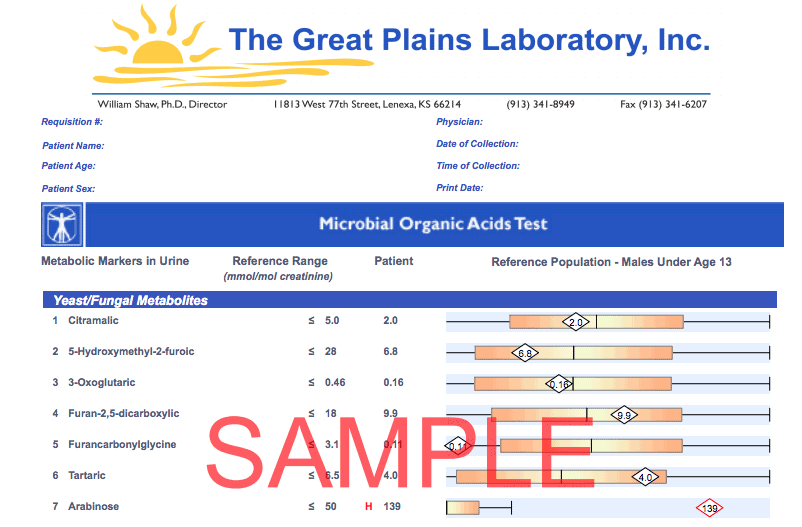
It can be helpful to know about oxalates, because oxalates feed Candida.
You get oxalates through eating high oxalate foods (beets, swiss chard, almonds, sweet potatoes, spinach, chocolate, rhubarb).
However, molds that have colonized the body also produce oxalates. This is why it can be helpful to look for oxalates as well.
Oxalates get stored in the tissues, so the oxalate testing only shows what’s being excreted. It doesn’t show what’s in the tissues
On rare occasions, someone will have obvious candida (athlete’s foot or toenail fungus and vaginal yeast infections), but it won’t show on the test.
This can be because there are many types of Candida. And 1 test can’t possibly test for all of them. But the test links above are the most comprehensive out there.
If you’ve tested positive or have really obvious candida symptoms, it’s time to get to work.
(Everyone is different. The information and supplements in this blog are for informational and educational purposes. They are not meant to substitute for medical advice. None of the information in this blog post is meant for diagnostic or treatment purposes. Always work with your healthcare provider and under the supervision of a medical practitioner)
I’ve put together some options for candida you can discuss with your healthcare practitioner. And I’ll share that with you in the next section.
Where To Start With Candida
If you’re wondering where to start, here are some ideas.
For my clients, I usually recommend supporting their bodies with a combo of these strategies. But, if there is Mold Toxicity, this gets addressed first.
Most people with Mast Cell Activation Syndrome or Histamine Intolerance do best increasing supplements very slowly – starting with sprinkles. Always listen to your body.
And please work with your health care practitioner. They can help customize it to your situation.
Remember, this is for informational and educational purposes only. These are not prescriptive or meant to treat, diagnose, or cure any disease or disorder.
1. Low Carb/Low Sugar/Low Fruit diet + No alcohol
This is the #1 place to start. For about 20-30% of people with Mast Cell Activation Syndrome or Histamine Intolerance, cleaning up the diet clears up candida.
Why is this? Because sugar feeds candida. Alcohol feeds candida. Starches feed candida.
And it doesn’t matter the source. Even fruit is very high in natural sugar that feeds candida as well.
So be sure to stop:
- Sugar
- Fruit
- Alcohol
- Refined grains (like white rice)
(Some people get ill when stopping carbs and sugar. If this is the case for you, it is very important you consult with your healthcare practitioner before lowering your carbs to find out why.
If you are on a limited number of foods already, be sure to work with a healthcare practitioner before you reduce foods further.)
2. Biotin
Biotin is an important B vitamin. And it can be really helpful with Candida.
This is because biotin keeps candida from changing into an invasive form of Candida. This invasive form is called a mycelial form.
This “mycelial” form punctures cells and then hangs on tight. It’s much harder to get rid of Candida in this form.
Some people have found taking 2,000-6,000 micrograms (2-6mg) of biotin per day can help.
I prefer this biotin:
3. Saccharomyces Boulardii
Saccharomyces Boulardii is a type of beneficial yeast. It naturally lives in our guts.
You can also take it as a probiotic species. It may help reduce candida overgrowth. It does this by outcompeting Candida.
Saccharomyces Boulardii even has been shown to help balance bacteria in the gut. And to help protect the gut lining.
And, it can bind the gliotoxin we were talking about earlier. Isn’t that cool?
It’s best taken with food.
If you have IgG or IgE Candida allergies, you may not tolerate it, though. But, other people do great with it. It really helped my gut.
(I don’t really like the popular Florastor® because it has lactose, unfortunately. Many people with Mast Cell Activation have milk allergies.)
This is my favorite Saccharomyces Boulardi:
4. Bentonite Clay
Bentonite clay has been used for hundreds of years. It’s been shown to be effective for detoxification of Gliotoxins produced by mold and likely Candida.
It’s very important to take it 1 hour before or 2 hours after meals, meds, or supplements.
This is because Bentonite can bind up minerals, supplements, and medications. This isn’t usually a problem if it’s taken away from these things.
Taking it near a snack is usually ok.
It is very important to use a clean source that has been microfiltered to remove heavy metals and other toxins.
I like Premier Research Lab’s Medi-Clay:
5. Undecylenic Acid
Undecylenic Acid is a fatty acid that comes from Castor oil. It has a lot of possible actions against Candida.
It’s been shown in research to reduce Candida growth. And it can help get rid of Candida biofilm.
But, it’s a powerful antifungal, so go SLOW!!
Thorne makes one of the best forms of Undecylenic Acid:
One downside to Undecylenic Acid is that you can’t open the capsule. This is because it’s an acid. And can be a little strong for your mouth tissues.
This is why they say to start with 1 whole capsule. But only try this if you are tolerating supplements well. (If not, check out our Mast Cell Nervous System Reboot.)
6. Monolaurrin
Monolaurin is another option against Candida. It is derived from coconut oil.
Studies have shown that monolaurin can break down the biofilms produced by candida. And help eliminate the infection.
It has also been shown in research to lower inflammation.
It’s a strong anti-viral. So, it’s important to go very slow with this.
I use this monolaurin:
7. Berberine
Berberine is a powerful antifungal that’s found in a variety of different herbs, such as barberry. It can also be found in Oregon grape and berberine has been shown in research to combat candida. And it can help the body clean up dead Candida cells.
This berberine is the one I like:
8. Nanoparticle Silver
Silver is an effective antimicrobial. It has been shown in research to kill off Candida.
Colloidal silver can build up in the body, causing silver toxicity. Which is why you don’t want to take that form.
And it’s also why I make sure to use nanoparticle silver instead. This form is too small to build up in the body. So, it can’t cause toxicity.
But it can still be powerful against Candida.
I find this nanoparticle silver works best:
9. Interfase Plus
Interfase Plus is a super biofilm buster supplement. It is strong!
Normally, this is the last thing I introduce when working on Candida or mold.
I recommend using caution with this one. And if you try it, go VERY slowly.
It kicked my butt the first time I tried it because I took too much. I had to take several months to taper up to 1 capsule.
It can be taken about 30 minutes before foods to keep it from being as strong.
This is Interfase Plus:
Again, it’s important to introduce supplements VERY slowly – start with tiny amounts. I never recommend starting with a whole capsule, unless it’s something like the SF722 where you can’t open the capsule.
And be sure to work with your healthcare practitioner.
If you aren’t tolerating any supplements, though, then don’t start here. These are the places to start:
Mast Cell Nervous System Reboot Course – this is for anyone who’s struggling with sensitivities to foods, supplements, medications, mold, chemicals, etc.
Top 8 Mast Cell Supporting Supplements Master Class – this class covers how to start supplements, the best 8 for beginners, and lots of tips for how to increase supplements slowly.
If you don’t tolerate these supplements, a few things may have happened:
- You kept eating sugar, fruit, carbs, and drinking alcohol
- You went too fast
- You didn’t introduce them in the right order
- You haven’t fully addressed your Haywire Mast Cell-Nervous System Wiring
- You may have Mold Toxicity
- You may have something else going on and need to work with a healthcare practitioner
I mentioned at the beginning of this protocol how it’s important to follow a Low Carb/Low Sugar/Low Fruit diet + No alcohol.
I want to talk a little bit more about the reason for this diet next.
Sugar, Carbs, and Candida
Conquering the sugar cravings and limiting the carbs is essential if you want to kick the candida.
(Definitely avoid this step if you have a medical condition that keeps you from reducing your carbs – like pregnancy, breastfeeding, young age, heme dysregulation, eating disorders, malnourishment, etc.)
But if you can, it’s especially important if you have Mast Cell Activation Syndrome or Histamine Intolerance.
Sugar isn’t good for those with Mast Cell Activation Syndrome or Histamine Intolerance. That’s because elevated insulin triggers mast cells.
Besides that, sugar, carbs, and fruit feed candida. And that also applies to other fungal species, like mold.
So, you want to eat clean with low sugar, avoid fruit, and avoid simple carbs.
Simple carbs include:
- Sugar (even raw sugar)
- Coconut sugar and nectar
- Corn syrup
- Agave
- Maple syrup
- Honey
- Milk
- Beer
- White rice and other refined grains
- And many more
This doesn’t mean you have to do a full keto diet. In fact, full keto can actually feed candida.
The main takeaway here is to avoid simple carbs, sugars, and alcohol.
You can certainly keep the complex carbohydrates, like vegetables, sorghum, and other healthy sources of fiber and starch.
This is a crucial step. But it will rarely get rid of candida on its own.
You’re likely going to have to add certain targeted supplements to get rid of candida.
However, there are certain common candida treatments you may need to avoid if you have Mast Cell Activation Syndrome or Histamine Intolerance.
Common Candida Recommendations You May Want to Avoid
Some common foods and supplements that are recommended for candida include: clove, cinnamon, fermented vegetables, bone broth, and yogurt.
But these are going to be a problem if you have Mast Cell Activation Syndrome or Histamine Intolerance. Here’s why:
- Clove and Cinnamon are both high histamine spices. Using these as seasonings, tinctures, essential oils, or supplements are going to do more harm than good.
- Fermented veggies, and all other aged and fermented foods, are known to be high in histamine.
- Bone Broth is high in histamine and can increase oxalates.
- Yogurt is a fermented dairy (or nut milk) product that usually contains mast cell activating bacterial species and additives.
Now, you can make meat broth instead of bone broth.
To make meat broth, boil meat in water with desired veggies and herbs for 20-30 minutes. Freeze any leftovers right away.
This will still get some of the great healing effects, without the drawbacks when you have Mast Cell Activation Syndrome or Histamine Intolerance.
Now, what about medications that are used to treat candida? These can also be a problem for those of us with Mast Cell Activation Syndrome or Histamine Intolerance.
What To Know About Medications and Chronic Candida Infections
Again, this is for educational and informational purposes only – please work with your health care practitioner! This is in no way meant to be prescriptive or considered as treatment recommendations.
Candida has become more and more resistant to herbs – as have our gut bacteria.
So, sometimes people need prescription antifungals. This can especially be true when there is also Mold Toxicity.
Before I go into the prescription medications, I want to mention one thing:
It can be very helpful to have Saccharomyces Boulardi and Bentonite Clay on board before starting antifungal medications, if tolerated.
This can help to reduce the die-off effects (more below).
Nystatin – This is a prescription antifungal. It is often better compounded for those with Mast Cell Activation Syndrome. This is because of dyes and fillers in the regular version.
The regular Nystatin has FD&C colors, lactose, cornstarch and titanium dioxide. This is why I’ve always gotten it compounded.
Nystatin doesn’t absorb well and doesn’t affect the liver. This is why it is usually considered the safest medication for Candida.
But it’s sometimes needed for 6 to even 12 months in very stubborn cases. Especially where there has been Mold Toxicity…
Diflucan – This is another antifungal medication. It is also best if compounded for those with Mast Cell Activation Syndrome. This is because of dyes and fillers in it too.
The regular Diflucan has FD&C colors, aluminum lake dye, citric acid, and titanium dioxide.
It can be hard on the liver and thyroid when taken daily for extended time.
Some practitioners have found it can be more effective when taken 1x every 2 weeks.
This is because candida can feel threatened by the Diflucan. Then it can start shifting forms and become even more resistant.
Pulsing it every 2 weeks is thought to help avoid Candida becoming more resistant. This kind of pulsing is often safer as well.
Always work with a medical practitioner on medications and follow your prescribers directions.
These medications can cause massive die off, making people feel bad…
Below, I’ll cover things to know if you have mast cell issues.
Die Off and Candida
Die Off can happen when killing Candida. First of all, what is Die Off?
“Die Off” happens when candida dies from added medication, supplements, or starving it by stopping sugar, alcohol, and refined carbs.
When Candida is killed off, it releases toxins. If this happens too fast, it can cause you to feel terrible.
Some Common Die Off Reaction Symptoms include the following:
- Headache, migraines
- Changes in bowel movements – constipation and/or diarrhea
- Fatigue
- Flu-like symptoms, muscle aches, feeling bad all over
- Chills, mild-moderate fever (99-102.5)
- Nausea, vomiting
- Presence of mucous and/or some blood in your stool
- Brain fog/decreased concentration, irritability
- Rash
It’s very important that you DON’T Push Through Die Off if you have Mast Cell Activation Syndrome or Histamine Intolerance – You can set off a mast cell cascade that can last weeks to months.
It’s MUCH better to go slow and take your time. Unless your practitioner is concerned about serious health issues that need to be addressed aggressively.
If you do get reactions, Here’s What May Help:
- Pause what provoked the die off until symptoms calm back down (like a supplement). Then restart more slowly.
- Drink extra water. Add lemon to water if tolerated (1/4 to ½ squeezed lemon)
- Use a little Bicarb formula.
Bicarbs can help calm down reactions. This is like taking baking soda. Except it also has a little Potassium Bicarbonate as well that I find helpful.It’s important not to exceed the number of capsules on the bottle.
This is the one I use:
- Increase DAO supplements, if tolerated and approved by your health care practitioner
- Increase other tolerated mast cell/histamine support supplements, if approved by your healthcare practitioner
- Do gentle lymph draining techniques, as tolerated:
- Gentle walking
- Rebounding
- Heel drops (inhale and lift up on toes, exhale and gently drop heels to floor)
- Nap and sleep more than usual
- Reduce stress and preserve energy
- Eat very cleanly and go lower histamine
- Work on Nervous System Supports from the Mast Cell Nervous System Reboot
The Bottom Line
Remember that Candida is naturally found in your gut. And the right Candida balance is very important.
If Candida gets out of balance, it can trigger more Mast Cell Activation Syndrome.
And Mold Toxicity is one of the major underlying causes of stubborn Candida.
There are many ways to work on Candida overgrowth. AND at the same time, keep it low histamine and keep those mast cells happy.
Be sure to work with your healthcare practitioner on finding options that are right for you.
Mast Cell Nervous System Reboot Course – this is for anyone who’s struggling with sensitivities to foods, supplements, medications, mold, chemicals, etc.
*Some links in this website are affiliate links, which means Mast Cell 360 may make a very small commission if you purchase through the link. It never costs you any more to purchase through the links, and we try to find the best deals we can. We only recommend products that we love and use personally or use in the Mast Cell 360 practice. Any commissions help support the newsletter, website, and ongoing research so Mast Cell 360 can continue to offer you free tips, recipes, and info. Thank you for your support!
References
Aggor, F., Way, S. S., & Gaffen, S. L. (2019). Fungus Among Us: The Frenemies Within. Trends in immunology, 40(6), 469–471. https://doi.org/10.1016/j.it.2019.04.007
Bertling, A., Niemann, S., Uekötter, A., Fegeler, W., Lass-Flörl, C., von Eiff, C., & Kehrel, B. E. (2010). Candida albicans and its metabolite gliotoxin inhibit platelet function via interaction with thiols. Thrombosis and haemostasis, 104(2), 270–278. https://doi.org/10.1160/TH09-11-0769
Bonhomme, J., Chauvel, M., Goyard, S., Roux, P., Rossignol, T., & d’Enfert, C. (2011). Contribution of the glycolytic flux and hypoxia adaptation to efficient biofilm formation by Candida albicans. Molecular microbiology, 80(4), 995–1013. https://doi.org/10.1111/j.1365-2958.2011.07626.x
Casanova, M., Lopez-Ribot, J. L., Martinez, J. P., & Sentandreu, R. (1992). Characterization of cell wall proteins from yeast and mycelial cells of Candida albicans by labelling with biotin: comparison with other techniques. Infection and immunity, 60(11), 4898–4906. https://doi.org/10.1128/IAI.60.11.4898-4906.1992
Cernáková, M., & Kostálová, D. (2002). Antimicrobial activity of berberine–a constituent of Mahonia aquifolium. Folia microbiologica, 47(4), 375–378. https://doi.org/10.1007/BF02818693
Chang, Y., Gu, W., & McLandsborough, L. (2012). Low concentration of ethylenediaminetetraacetic acid (EDTA) affects biofilm formation of Listeria monocytogenes by inhibiting its initial adherence. Food microbiology, 29(1), 10–17. https://doi.org/10.1016/j.fm.2011.07.009
de Almeida, J., Hoogenkamp, M., Felippe, W. T., Crielaard, W., & van der Waal, S. V. (2016). Effectiveness of EDTA and Modified Salt Solution to Detach and Kill Cells from Enterococcus faecalis Biofilm. Journal of endodontics, 42(2), 320–323. https://doi.org/10.1016/j.joen.2015.11.017
De Zuani, M., Paolicelli, G., Zelante, T., Renga, G., Romani, L., Arzese, A., Pucillo, C., & Frossi, B. (2018). Mast Cells Respond to Candida albicans Infections and Modulate Macrophages Phagocytosis of the Fungus. Frontiers in immunology, 9, 2829. https://doi.org/10.3389/fimmu.2018.02829
Ghio, A. J., Peterseim, D. S., Roggli, V. L., & Piantadosi, C. A. (1992). Pulmonary oxalate deposition associated with Aspergillus niger infection. An oxidant hypothesis of toxicity. The American review of respiratory disease, 145(6), 1499–1502. https://doi.org/10.1164/ajrccm/145.6.1499
Goggin, R., Jardeleza, C., Wormald, P. J., & Vreugde, S. (2014). Colloidal silver: a novel treatment for Staphylococcus aureus biofilms?. International forum of allergy & rhinology, 4(3), 171–175. https://doi.org/10.1002/alr.21259
Hogan, S., O’Gara, J. P., & O’Neill, E. (2018). Novel Treatment of Staphylococcus aureus Device-Related Infections Using Fibrinolytic Agents. Antimicrobial agents and chemotherapy, 62(2), e02008-17. https://doi.org/10.1128/AAC.02008-17
Jalal, M., Ansari, M. A., Alzohairy, M. A., Ali, S. G., Khan, H. M., Almatroudi, A., & Siddiqui, M. I. (2019). Anticandidal activity of biosynthesized silver nanoparticles: effect on growth, cell morphology, and key virulence attributes of Candida species. International journal of nanomedicine, 14, 4667–4679. https://doi.org/10.2147/IJN.S210449
Johannessen, L. N., Nilsen, A. M., & Løvik, M. (2005). The mycotoxins citrinin and gliotoxin differentially affect production of the pro-inflammatory cytokines tumour necrosis factor-alpha and interleukin-6, and the anti-inflammatory cytokine interleukin-10. Clinical and experimental allergy : journal of the British Society for Allergy and Clinical Immunology, 35(6), 782–789. https://doi.org/10.1111/j.1365-2222.2005.02249.x
Kelesidis, T., & Pothoulakis, C. (2012). Efficacy and safety of the probiotic Saccharomyces boulardii for the prevention and therapy of gastrointestinal disorders. Therapeutic advances in gastroenterology, 5(2), 111–125. https://doi.org/10.1177/1756283X11428502
Lee, S. H., Barnes, W. G., & Schaetzel, W. P. (1986). Pulmonary aspergillosis and the importance of oxalate crystal recognition in cytology specimens. Archives of pathology & laboratory medicine, 110(12), 1176–1179.
Lewith, G. T., Chopra, S., Radcliffe, M. J., Abraham, N., Prescott, P., & Howarth, P. H. (2007). Elevation of Candida IgG antibodies in patients with medically unexplained symptoms. Journal of alternative and complementary medicine (New York, N.Y.), 13(10), 1129–1133. https://doi.org/10.1089/acm.2007.0568
Lopes, J. P., Stylianou, M., Nilsson, G., & Urban, C. F. (2015). Opportunistic pathogen Candida albicans elicits a temporal response in primary human mast cells. Scientific reports, 5, 12287. https://doi.org/10.1038/srep12287
Loewus FA, Saito K, Suto RK, Maring E. Conversion of D-arabinose to D-erythroascorbic acid and oxalic acid in Sclerotinia sclerotiorum. Biochem Biophys Res Commun. 1995 Jul 6;212(1):196-203. doi: 10.1006/bbrc.1995.1956. PMID: 7612007.
Mathur, S., Goust, J. M., Horger, E. O., 3rd, & Fudenberg, H. H. (1977). Immunoglobulin E anti-Candida antibodies and candidiasis. Infection and immunity, 18(1), 257–259. https://doi.org/10.1128/IAI.18.1.257-259.1977
Mionić Ebersold, M., Petrović, M., Fong, W. K., Bonvin, D., Hofmann, H., & Milošević, I. (2018). Hexosomes with Undecylenic Acid Efficient against Candida albicans. Nanomaterials (Basel, Switzerland), 8(2), 91. https://doi.org/10.3390/nano8020091
Monteiro, D. R., Gorup, L. F., Silva, S., Negri, M., de Camargo, E. R., Oliveira, R., Barbosa, D. B., & Henriques, M. (2011). Silver colloidal nanoparticles: antifungal effect against adhered cells and biofilms of Candida albicans and Candida glabrata. Biofouling, 27(7), 711–719. https://doi.org/10.1080/08927014.2011.599101
Muntz F. H. (1999). Oxalate-producing pulmonary aspergillosis in an alpaca. Veterinary pathology, 36(6), 631–632. https://doi.org/10.1354/vp.36-6-631
Neag, M. A., Mocan, A., Echeverría, J., Pop, R. M., Bocsan, C. I., Crişan, G., & Buzoianu, A. D. (2018). Berberine: Botanical Occurrence, Traditional Uses, Extraction Methods, and Relevance in Cardiovascular, Metabolic, Hepatic, and Renal Disorders. Frontiers in pharmacology, 9, 557.
Nobile, C. J., & Johnson, A. D. (2015). Candida albicans Biofilms and Human Disease. Annual review of microbiology, 69, 71–92. https://doi.org/10.1146/annurev-micro-091014-104330
Richter, K., Facal, P., Thomas, N., Vandecandelaere, I., Ramezanpour, M., Cooksley, C., Prestidge, C. A., Coenye, T., Wormald, P. J., & Vreugde, S. (2017). Taking the Silver Bullet Colloidal Silver Particles for the Topical Treatment of Biofilm-Related Infections. ACS applied materials & interfaces, 9(26), 21631–21638. https://doi.org/10.1021/acsami.7b03672
Ruijter, G., van de Vondervoort, P., & Visser, J. (1999). Oxalic acid production by Aspergillus niger: an oxalate-non-producing mutant produces citric acid at pH 5 and in the presence of manganese. Microbiology (Reading, England), 145 ( Pt 9), 2569–2576. https://doi.org/10.1099/00221287-145-9-2569
Piliponsky, A. M., & Romani, L. (2018). The contribution of mast cells to bacterial and fungal infection immunity. Immunological reviews, 282(1), 188–197. https://doi.org/10.1111/imr.12623
Seleem, D., Chen, E., Benso, B., Pardi, V., & Murata, R. M. (2016). In vitro evaluation of antifungal activity of monolaurin against Candida albicans biofilms. PeerJ, 4, e2148. https://doi.org/10.7717/peerj.2148
Shao, T. Y., Ang, W., Jiang, T. T., Huang, F. S., Andersen, H., Kinder, J. M., Pham, G., Burg, A. R., Ruff, B., Gonzalez, T., Khurana Hershey, G. K., Haslam, D. B., & Way, S. S. (2019). Commensal Candida albicans Positively Calibrates Systemic Th17 Immunological Responses. Cell host & microbe, 25(3), 404–417.e6. https://doi.org/10.1016/j.chom.2019.02.004



This is incredibly helpful and not good news, though I’ve known I’ve been eating a diet, which is not the best for my diagnoses of systemic mold, candida, & fungus.
I do have MAST CELL activation syndrome and histamine intolerance… along autoimmune challenges.
I do believe there are a lot of anti-nutrients in some veggies and other things like nuts, legumes, and grains…
I have been running away from mold toxic housing for years…that is what got me off quilter in the 1st place.
You are my go to as far as the histamine issues etc.
I see that I’ve been dealing with getting oxalates out of my diet as well. I’m pretty good about the low histamine foods… but, I do eat a high starch diet & fruit… Given I can’t digest animal protein … it constipated me and I’ve tried everything to remedy that on going issue no matter what I eat. I wish I could consult with someone such as yourself…however I am a lucky recipient of disability because of my compromised health.
Do you have any dietary suggestions for us with candida etc?
Thank you for all the info you share…it is such a gift!!!
And it is much appreciated.
Hi Saragrace,
Toward the end of the article, Beth has listed some dietary tips, more in depth, but the basic things to avoid are:
Sugar, Fruit, Alcohol, Refined grains (like white rice)
You can keep the complex carbohydrates like vegetables, sorghum, and other healthy sources of fiber and starch.
Thank you so much for this thorough article. I have found molybdnum really useful when dealing with the drunk/disoriented feelings that can accompany excessive die-off. Have you ever had luck with this, or is there a reason you do not recommend it?
Hi Amy,
Yes, it’s very helpful for some people, and I’m so glad to hear it works for you! It’s not always well tolerated, so it needs more discussion than we could add to this blog, but we might be able to do a separate blog about it.
For anyone looking for molybdenum, here’s the one I use for myself and recommend to some clients (remember to check things out for yourself, if you want to try it):
https://us.fullscript.com/product_cards/58785/redirect?store_slug=mastcell360
Beth
Hi Beth. Great post. Can you provide references for the research on oxalates feeding candida? I have issues with both and would like more information on the connection.
Thanks.
Anita
Hi Anita,
This study looked at candida responses when exposed to oxalates: Bonhomme, J., Chauvel, M., Goyard, S., Roux, P., Rossignol, T., & d’Enfert, C. (2011). Contribution of the glycolytic flux and hypoxia adaptation to efficient biofilm formation by Candida albicans. Molecular microbiology, 80(4), 995–1013. https://doi.org/10.1111/j.1365-2958.2011.07626.x
Hi Beth,
What is your view of using colonics to decrease fungus, bacteria and parasites in the colon? Also using diatomaceous earth? My son has major problems with salicylate sensitivity. (Amazingly his major OCD has gone to almost zero, by recently eliminating salicylates in his diet/personnel products.) However this greatly eliminates the products he can use for an anti-fungal. He also has an auto-immune disease. (and of course has histamine and oxalate problems and a very sick gut). I am viewing colonics because he goes into major herxing stress with even a little anti-fungal products. Thanks in advance.
Hi Pat,
Beth says “Colonics are tricky, so it’s really case by case. Diatomaceous earth can be harsh on the intestines so I rarely recommend it.”
Some other resources which might be helpful if your son is herxing with antifungals are her Master Classes which can be found here:
Nervous system support: https://mastcell360.com/mastcell-reboot/
Top 8 Mast Cell Supporting Supplements course: https://mastcell360.com/master-class/
and these articles she wrote about addressing Mold toxins: https://mastcell360.com/category/mold/
In your opinion, is it okay to put potato or sweet potato starch in my soups in order to avoid going too low carb while on the anti-candida diet? (I have a confirmed systemic candida infection.).
Hi Emily,
Specific dietary requirements are best addressed when working 1:1 with a practitioner. This really depends on your case.
This is so incredibly helpful!! Thank you!!
I’m doing many of these things but may have increased SF722 too quickly. I’m super excited to hear that berberine may help clear up the dead candida and bentonite clay can help with the toxins. And I appreciate the suggestions for the bicarb for calming things down.
Hi Elizabeth, we are happy to hear you found this post helpful!
This is a very informative site, definitely one of the better ones out there for candida.
I‘be been struggling for years now after taking some really strong antibiotics. I have yeast and mast cell issues as well as histamine intolerance and extreme sensitivity to many foods. I took sf722 for a couple of months and developed extreme anxiety which I read was due to my histamine intolerance. I was waking up almost every night with severe panic attacks. It took over a month to subside after I stopped taking the supplement.
What should be my next course of action?
Hi Joe! Unfortunately, since we are unfamiliar with your individual case, we are unable to answer a personalized medical question regarding your next steps for treating candida specifically. At Mast Cell 360, our practitioners work extensively with clients getting to know their medical history, their genetics, their diet, and so much more. This helps make sure that our clients are getting focused care. Although I can say that one of the first steps for clients, especially when having multiple sensitivities to many foods, is to work on calming the nervous system. You might be interested in our Nervous System Reboot course, which you can learn more about here: https://mastcell360.com/mastcell-reboot/